Walk into a rural emergency department at 2 a.m. and the scene often looks nothing like what you see in urban teaching hospitals. One physician. Two nurses. A respiratory therapist on call who lives thirty minutes away. A crash cart with medications that were last audited six months ago. When a cardiac arrest rolls through the door, every member of that lean team has to perform at an extraordinarily high level because there is no backup trauma bay down the hall, no rapid response team to call, and no cardiologist available to take over.
Rural emergency departments serve roughly 20 percent of the U.S. population but operate with a fraction of the specialty resources available in metropolitan hospitals. According to data from the Rural Health Information Hub, rural health care systems face persistent shortages of specialists, limited infrastructure, and significant financial constraints that translate directly into longer wait times, fewer monitoring capabilities, and more frequent patient transfers. For a cardiac arrest patient, time is muscle and brain tissue. Every minute without effective Advanced Cardiovascular Life Support intervention reduces the probability of a favorable neurological outcome.
The good news is that maximizing ACLS outcomes in a resource-limited rural setting is absolutely achievable. It requires deliberate preparation, smart use of technology, strong team dynamics, and a commitment to ongoing training that does not demand clinicians leave their communities for expensive, time-consuming courses. This guide was written by practicing emergency medicine physicians who have worked in exactly these environments, and it outlines practical, evidence-based strategies that rural ED teams can implement starting today.
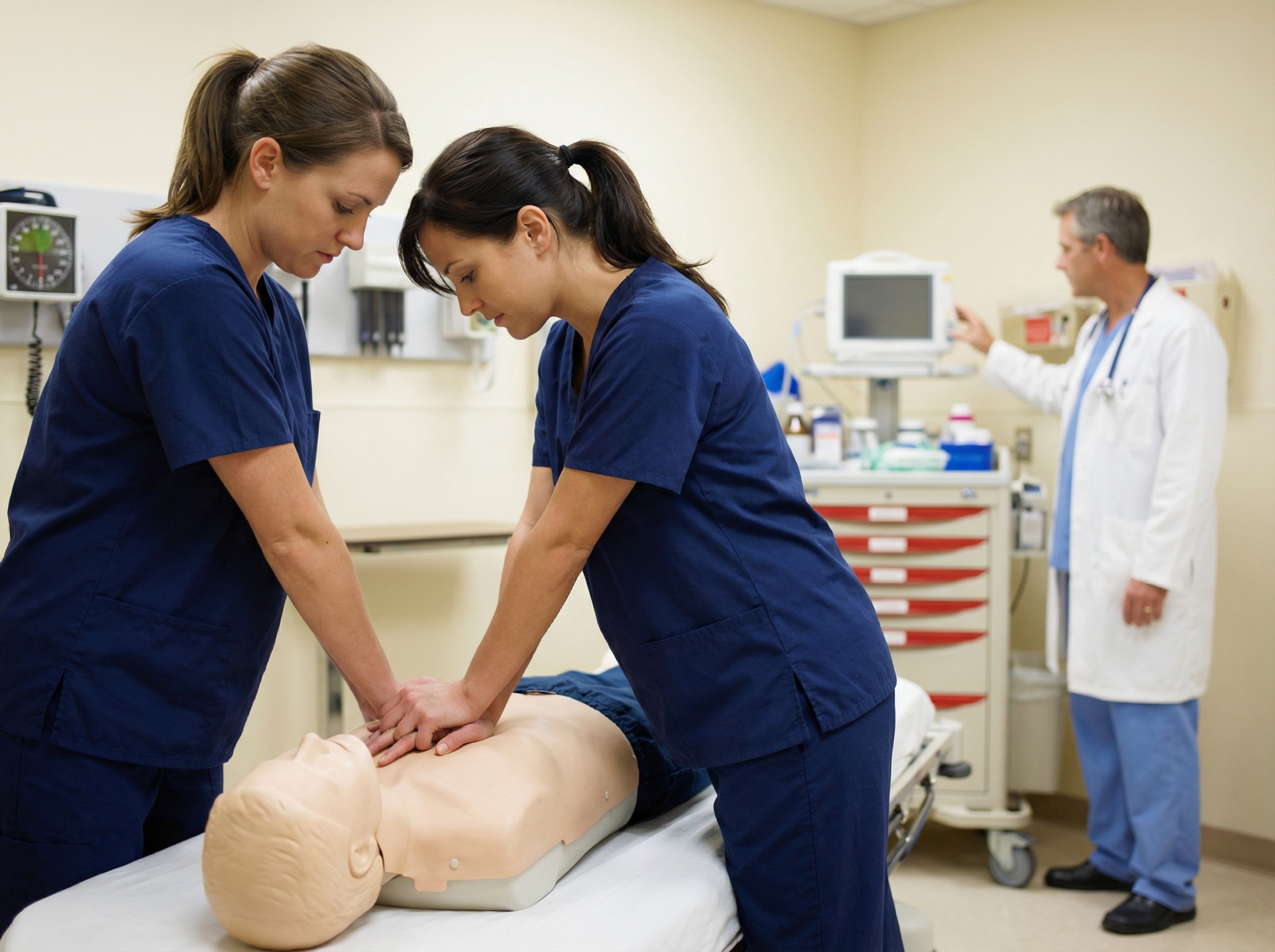
Before identifying solutions, it helps to understand the scope of the problem. Research summarized by the National Institutes of Health confirms that patients experiencing out-of-hospital cardiac arrest in rural areas have lower odds of achieving return of spontaneous circulation at emergency department arrival compared to patients in urban areas. The disparity is not primarily a matter of clinical knowledge. It is a systems problem. Response times are longer. Bystander CPR rates are lower. Post-resuscitation capabilities such as targeted temperature management and coronary catheterization are less accessible.
A systematic review and meta-analysis published in Resuscitation confirmed that rurality poses unique challenges to out-of-hospital cardiac arrest management across every phase of the chain of survival. Rural communities also experience higher rates of certain cardiac risk factors including obesity, tobacco use, and limited access to preventive cardiology, which means the patients arriving in these emergency departments are often higher acuity at baseline.
None of this is meant to be discouraging. It is context. When you understand where the gaps exist, you can target your interventions precisely. And the most high-yield intervention available to any rural ED is ensuring every member of the team has deep, current ACLS knowledge they can execute under pressure, without hesitation.
In urban systems, sending a nurse to an all-day ACLS renewal course creates a minor inconvenience. In a rural critical access hospital, that same absence can mean pulling a staff member from the only available shift, leaving a department dangerously understaffed. Traditional in-person ACLS certification courses were designed for a healthcare environment that does not reflect the operational reality of rural emergency medicine.
Online ACLS certification has changed this calculus entirely. Platforms built by practicing emergency physicians allow rural clinicians to complete their certification or recertification on their own schedule, whether that is during a quiet overnight shift, between patients on a slow afternoon, or at home after a double shift. For a department where scheduling flexibility is not a luxury but a survival requirement, this matters enormously.
When evaluating online ACLS options for your department, look for platforms that are based on current AHA and ILCOR guidelines, developed by clinically active emergency medicine physicians, and accepted by your credentialing body and hospital system. Affordable ACLS was built specifically by Board Certified Emergency Medicine physicians who recognized that busy clinicians needed a more practical recertification pathway. At $89 for ACLS recertification and $99 for initial certification, cost is not a barrier even for departments operating on tight budgets. For teams looking to certify multiple staff members simultaneously, group certification solutions can reduce per-person costs further while keeping your entire team current.
The core ACLS algorithms do not change based on your hospital's budget or location. High-quality CPR, early defibrillation, and systematic identification and treatment of reversible causes remain the pillars of successful resuscitation regardless of setting. What changes in a rural environment is how you operationalize those algorithms when resources are constrained.
The Hs and Ts framework for identifying reversible causes of cardiac arrest is arguably more important in rural settings than anywhere else. Without immediate access to advanced diagnostics, your clinical reasoning has to do more of the work. Hypovolemia, hypoxia, hydrogen ion excess, hypo- and hyperkalemia, and hypothermia are all potentially reversible with resources most rural EDs have available. Tension pneumothorax and tamponade can be addressed at bedside. Thrombosis, both pulmonary and coronary, requires coordination with tertiary referral systems. Understanding which of the Hs and Ts you can treat versus which require transfer is an essential part of rural ACLS decision-making.
Medication management is another area where rural EDs need deliberate preparation. ACLS pharmacology is specific and time-sensitive. Knowing your epinephrine dosing, amiodarone protocols, and adenosine administration by memory is not optional in an environment where you may be the only physician present. An ACLS medications reference posted in the crash cart area and internalized through regular review can be the difference between a confident team executing a resuscitation and a team paralyzed by uncertainty. Similarly, mastery of the adult cardiac arrest circular algorithm ensures your team cycles through interventions systematically rather than reactively.
One of the counterintuitive advantages of rural emergency departments is that small teams often develop tighter cohesion than large hospital systems where staff rotates constantly. A core team of six to eight providers who work together regularly and train together deliberately can achieve resuscitation performance that rivals much larger departments. The key is structuring that familiarity into explicit role assignments and communication protocols.
Effective ACLS team dynamics require a designated team leader, clear closed-loop communication, and role assignments established before a code begins, not during it. In a rural ED, this means posting laminated role assignment cards near the crash cart, running through assignments at the start of each shift when team composition changes, and ensuring every clinician knows both their primary role and at least one backup role in case a team member is unavailable. The communication scripts and team dynamics frameworks built into ACLS training exist precisely because human performance degrades under acute stress and explicit protocols prevent critical errors.
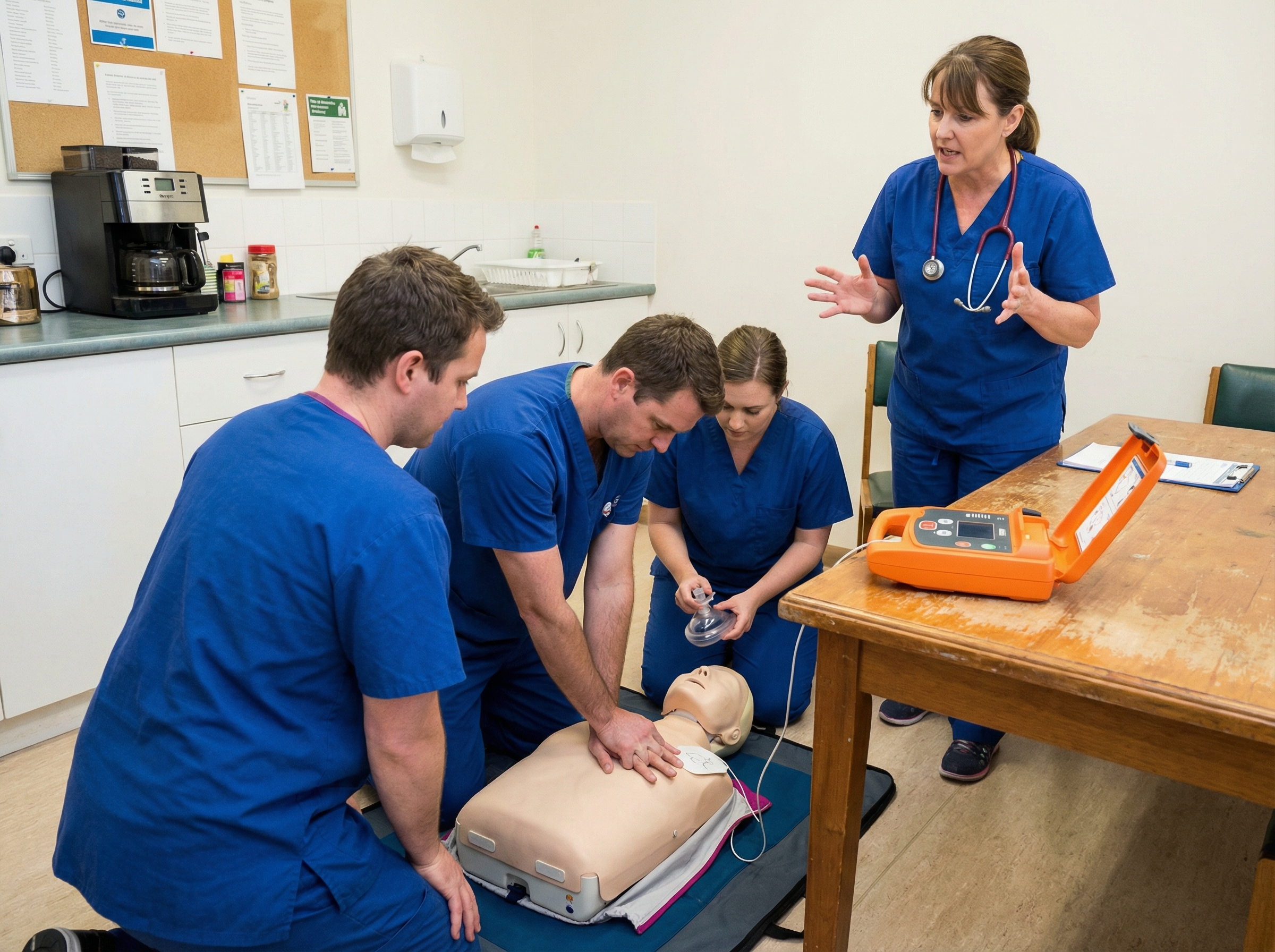
New members of rural emergency teams face a particular challenge because the smaller team size means they are expected to perform at a high level with less ramp-up time. Building confidence before a real code is essential. Regular simulation exercises, even low-fidelity scenarios using a mannequin in a break room, create the muscle memory and cognitive familiarity that determines performance under pressure. For newer providers joining a rural code team, structured frameworks for building confidence can accelerate the learning curve significantly.
Urban teaching hospitals often have dedicated simulation centers with high-fidelity mannequins, video debriefing systems, and simulation educators on staff. Rural emergency departments have none of that. What they do have is something equally powerful: a small, consistent team and real clinical cases to debrief after every critical event.
Effective simulation in a resource-limited setting does not require expensive equipment. A basic CPR mannequin, a defibrillator trainer, and a facilitator who can run a structured scenario are sufficient to conduct meaningful practice. Monthly code drills that rotate different team configurations, emphasize role clarity, and practice the full resuscitation sequence from initial response through post-arrest care build the kind of automaticity that saves lives. Research on simulation training demonstrates that the benefits extend far beyond skill acquisition into the domain of team communication and stress inoculation. As discussed in depth by our guide on simulation training and real-world resuscitation skills, even low-fidelity practice produces measurable improvements in clinical performance.
Post-event debriefing is equally important and equally underutilized in rural settings. After every resuscitation attempt, a structured ten-minute debrief that identifies what went well, what could be improved, and what system changes are needed converts clinical experience into institutional learning. This practice costs nothing and compounds over time into a culture of continuous improvement that systematically closes the gap between current and optimal ACLS performance. For additional guidance on structuring these conversations, the role of debriefing after ACLS events is a resource every rural ED leader should review.
One of the most significant developments in rural emergency medicine over the past decade is the expansion of telemedicine infrastructure that allows rural providers to access specialist expertise in real time. For ACLS scenarios, this means a rural physician managing a complex post-arrest patient can have a cardiologist or critical care specialist providing guidance via video within minutes, without waiting for a transfer that might take hours.
According to research published by the National Institutes of Health on telemedical direction in rural EMS systems, tele-emergency medicine connects providers at central hub emergency departments to small rural hospitals through video technology, allowing advanced life support-level guidance to reach communities that could not otherwise access it. For cardiac arrest management, this translates into real-time guidance on ACLS algorithm progression, medication decisions, and post-resuscitation care planning.
The U.S. Department of Health and Human Services telehealth guidance for emergency departments outlines implementation frameworks for rural hospitals considering tele-emergency medicine programs. The investment in connectivity infrastructure frequently pays for itself through reduced unnecessary transfers and improved outcomes on high-acuity cases. For rural departments already equipped with basic telehealth capabilities, integrating telemedicine into ACLS training workflows is a logical next step that extends both training access and real-time clinical support.
Rural emergency departments cannot always have every piece of equipment available in a level one trauma center. But they can ensure that the equipment they do have is meticulously maintained, immediately accessible, and operated by staff who have practiced with it regularly. A defibrillator that nobody has trained on is only marginally better than no defibrillator at all.
Crash cart standardization is a high-yield, low-cost intervention. Every rural emergency department should have a standardized crash cart layout that never changes, a daily or shift-based checklist system, and a medication restocking protocol that ensures critical ACLS drugs are always present and within expiration. The cognitive burden of a resuscitation is high enough without providers searching for equipment in unfamiliar locations or discovering mid-code that a medication is missing.
AED placement and maintenance deserve specific attention in rural settings where the ED may be the primary resource for the surrounding community. Understanding the full scope of AED capabilities, including pediatric settings, rhythm analysis limitations, and integration with manual defibrillation workflows, is essential for rural teams. A thorough understanding of AED use for adults and children should be part of every rural ED provider's foundational knowledge base.
Achieving return of spontaneous circulation is not the finish line. Post-cardiac arrest care is a complex, resource-intensive phase of management where many rural EDs face their greatest limitations. Targeted temperature management, continuous cardiac monitoring, hemodynamic optimization, and early coronary angiography for appropriate patients all require capabilities that may not exist at a critical access hospital.
The rural emergency physician's role in this phase is twofold: providing the best stabilization possible with available resources while simultaneously coordinating transfer to a facility with post-arrest management capabilities. This requires pre-established transfer protocols, relationships with receiving hospitals, and clear communication frameworks that transfer clinical responsibility efficiently without gaps in care. Regional referral systems are emerging as the most effective structural solution to rural post-arrest care limitations, as highlighted in current literature on in-hospital cardiac arrest management from npj Cardiovascular Health.
Within the rural ED, focusing on the elements of post-arrest care that are universally available makes the most impact. Airway management and ventilation optimization, hemodynamic support with available vasopressors, identification and treatment of obvious precipitating causes, and early 12-lead ECG interpretation for STEMI recognition are all achievable with standard rural ED resources. Mastery of bag-mask ventilation technique is particularly important in rural settings where definitive airway management may be delayed or complicated by limited available hands.
ACLS guidelines are updated regularly by the American Heart Association based on evolving evidence. For rural providers already stretched thin by clinical demands, keeping up with guideline changes is a real challenge. But guideline adherence directly affects patient outcomes, and providers who are practicing on outdated protocols may be delivering suboptimal care without realizing it.
Online resources, including guideline summaries, peer-reviewed continuing medical education, and updated certification courses, bring current evidence directly to rural providers wherever they are practicing. A review of the key changes in ACLS guidelines for 2025 is an efficient way for any rural ED provider to ensure their practice reflects current standards without dedicating hours to reviewing full guideline documents.
Recertification cycles also provide structured touchpoints for guideline updates. Rather than viewing ACLS recertification as an administrative checkbox, rural ED leaders can use the certification cycle as a deliberate team education event. When an entire team recertifies within the same window, using the same guideline-based curriculum, it creates shared mental models and standardized protocols that improve code performance. Platforms that allow immediate recertification, unlimited practice retakes, and self-paced completion make it practical to align team recertification schedules without operational disruption.
The most important resource in any emergency department is not equipment or medications. It is a team culture that prioritizes preparation, continuous learning, and honest reflection on performance. Rural emergency departments that build this culture consistently outperform their resource levels because every team member arrives for every shift ready to perform at their highest capability.
Building this culture requires leadership commitment at the department director level, consistent investment in training even when budgets are tight, and a psychological safety environment where providers can acknowledge gaps in knowledge or performance without fear of reprisal. Real cases that did not go as planned, reviewed honestly through structured debriefs, are among the most powerful educational tools available. For examples of how ACLS competency makes measurable differences in real clinical situations, documented ACLS success cases provide both inspiration and concrete clinical lessons.
Rural emergency medicine has always demanded providers who can do more with less. The clinicians working in these settings are often among the most resourceful, adaptable, and genuinely committed providers in the profession. What they frequently lack is not skill or dedication but access to training systems designed for their operational reality. Online certification platforms built by emergency physicians, telemedicine infrastructure that connects rural teams to specialist expertise, and systematic team training protocols designed for small crews are closing this gap. The rural patients who depend on these teams deserve the same standard of ACLS care available in any urban center, and with the right preparation, that standard is achievable.
If you are leading a rural emergency department or serving as a clinical educator for a rural team, the following priorities will deliver the greatest return on your investment of time and resources.
Rural emergency medicine is hard. The resource constraints are real and the stakes are high. But with the right systems in place, the right training infrastructure, and a team culture built around continuous improvement, rural emergency departments can deliver ACLS outcomes that reflect the quality of their people, not the limitations of their budgets. The patients counting on these teams in their most vulnerable moments deserve nothing less.
Maximizing ACLS outcomes in rural emergency departments is not about acquiring resources you do not have. It is about systematically optimizing what you do have: a skilled, dedicated team that trains together, communicates clearly, and stays current with evidence-based protocols. The gap between rural and urban cardiac arrest outcomes is a systems problem, and it has systems solutions.
Online ACLS certification built by practicing emergency physicians, telemedicine infrastructure connecting rural teams to specialist expertise, deliberate team training with regular simulation and structured debriefs, and crash cart standardization protocols are all within reach for virtually any rural emergency department. These are not aspirational goals. They are practical steps that resource-constrained teams across the country are implementing right now to deliver better care to rural patients who have no other options.
The team you build, train, and lead in your rural emergency department is your most important ACLS resource. Invest in that team consistently, starting with ensuring every member has the knowledge base that current, evidence-based ACLS certification provides. Everything else follows from there.
.jpg)

