When a real cardiac arrest happens in your facility, there is no time to think about who grabs the crash cart, who starts compressions, or who calls for the defibrillator. Every second of hesitation has measurable consequences. Research published in Circulation: Cardiovascular Quality and Outcomes confirms that hospitals with structured, ongoing resuscitation training programs see dramatically better survival outcomes than those relying on annual certification alone. A well-designed mock code program is one of the most powerful tools a healthcare facility can implement to close the gap between knowing the protocols and executing them flawlessly under pressure.
Mock codes, also called code blue simulations or in situ resuscitation drills, recreate the conditions of a real cardiac arrest in your facility's actual clinical environment. Unlike traditional classroom-based ACLS training, mock codes test the entire system: the team, the equipment, the environment, and the communication structure. The evidence is striking. Studies have documented facilities achieving a 41% overall reduction in code blue events after implementing a regular mock code program, along with significant improvements in time to first compression, defibrillation, and medication delivery. If your facility does not yet have a structured mock code program, or if your current program is inconsistent, this guide will walk you through every step of building one that works.
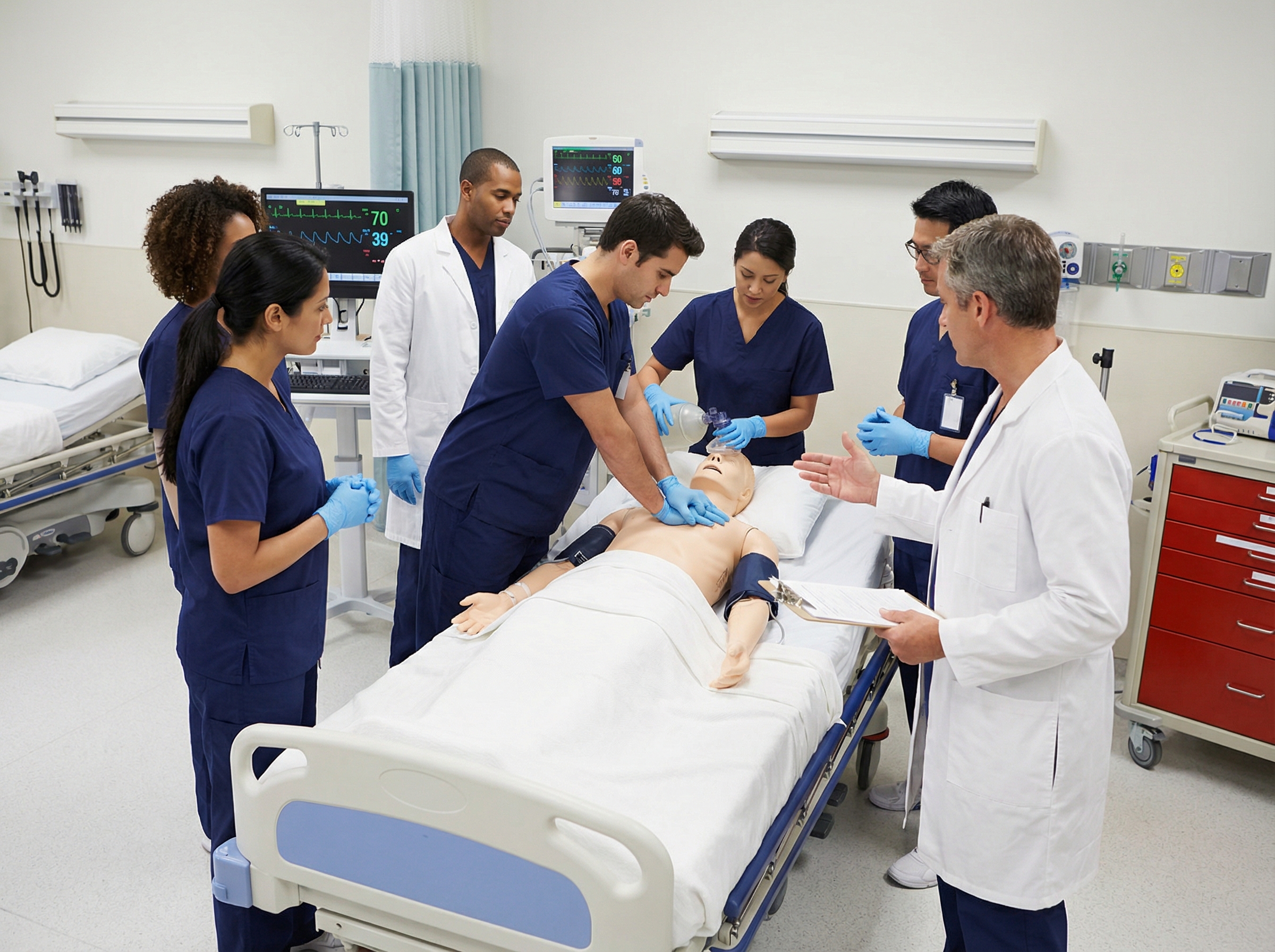
A mock code program is a systematic, recurring simulation-based training initiative in which healthcare teams respond to a staged cardiac arrest or other critical emergency scenario in their actual work environment. The scenario uses a high-fidelity manikin or a standardized patient actor placed in a real patient bed, with real equipment and real team members called to respond just as they would in an actual emergency.
Standard ACLS or BLS certification ensures that individual providers know the algorithms, medications, and technical skills required during a resuscitation event. That knowledge foundation is absolutely essential, and staying current with the latest ACLS guidelines is non-negotiable. However, certification alone does not guarantee that a team will perform well together in the chaos of a real code. Mock codes address the gap between individual knowledge and team performance by adding the critical element of applied practice in a realistic, high-stakes environment.
The research distinguishes between two primary types of mock codes: announced and unannounced. Announced drills give staff advance notice that a simulation will occur during a specific shift or time window, allowing for mental preparation. Unannounced drills, by contrast, more accurately replicate the surprise of a real event and provide a truer measure of team readiness. Most programs benefit from incorporating both types strategically throughout the year.
The case for mock code programs is not anecdotal. A robust body of peer-reviewed research supports simulation-based resuscitation training as one of the highest-yield educational interventions in clinical medicine. A systematic review and meta-analysis found statistically significant improvements across every measured outcome, including knowledge, process skill, product skill, and time-to-treatment. Perhaps most importantly, research documented measurable improvements in patient outcomes, with one study showing return of spontaneous circulation rates improving from 58.1% to 86.3% following implementation of a structured advanced resuscitation training curriculum.
A study examining longitudinal in situ mock code events and cardiac arrest skill performance found that regular drills produced lasting improvements and 100% compliance with achieving first compression within one minute, a benchmark directly correlated with survival. The American Heart Association now recommends in situ IHCA simulations as part of best practices for hospital resuscitation training, joining the National Academy of Medicine and The Joint Commission in that recommendation.
Understanding how simulation training enhances real-world resuscitation skills is fundamental to building a program with the right structure and frequency. The evidence consistently shows that low-dose, high-frequency training outperforms annual high-dose training when it comes to skill retention and team performance.
Every successful mock code program begins with the right people in charge. Your program director should be focused, organized, and detail-oriented, with strong clinical credibility and the interpersonal skills to engage staff across multiple departments. Depending on your facility size, this could be a physician champion, a nurse educator, or a quality improvement professional, ideally with simulation training experience or formal ACLS instructor credentials.
A steering committee broadens accountability and brings multiple perspectives to program design. Include representation from nursing, medicine, pharmacy, respiratory therapy, and hospital administration. Administrative support is not optional. Without leadership buy-in and protected time for training, even the most well-designed program will fail to achieve consistent participation.
Before designing your first drill, you need to understand your starting point. Review your facility's code data: response times, ROSC rates, survival to discharge, and code team performance metrics. Identify patterns in where errors or delays occur. Are compressions starting late? Is there confusion about team roles? Are medication errors happening because of poor communication?
Conduct a survey of staff confidence and knowledge. Providers who feel underprepared for code situations are more likely to hesitate, defer to others inappropriately, or perform technical skills incorrectly under stress. Building confidence as a code team member is an ongoing process that your mock code program directly supports. Use your baseline data to identify priority units and scenarios for your initial training calendar.
Effective mock code scenarios are grounded in the actual cases your team is most likely to encounter. Start by reviewing your facility's code data to identify the most common presenting rhythms, patient demographics, and clinical contexts. Develop a library of scenarios that includes ventricular fibrillation, pulseless ventricular tachycardia, PEA, and asystole. Include special circumstances such as the pregnant patient, the pediatric patient, respiratory arrest preceding cardiac arrest, and codes in procedural areas like the radiology suite or OR.
Each scenario should have a clear educational objective, a standardized patient presentation, a scripted progression, and predetermined decision points where the team's actions determine the scenario outcome. High-fidelity manikins that can display different cardiac rhythms, respond to defibrillation, and simulate physiological changes allow teams to practice the full ACLS algorithm from recognition through ROSC or termination of resuscitation. Reviewing the adult cardiac arrest circular algorithm with your team before and after scenarios reinforces the decision-making framework they will use in real events.
Frequency matters more than most program designers initially realize. The American Heart Association's Resuscitation Quality Improvement (RQI) program, now used by over 1,000 hospitals globally, is built on a low-dose, high-frequency model because research clearly shows that skills decay rapidly after training. Annual certification captures a snapshot of competence at one point in time; it does not maintain performance.
For most facilities, a practical starting point is quarterly mock codes per unit, with higher-acuity units such as the ICU, emergency department, and cardiac care units scheduling monthly drills. Build your schedule around shift patterns to ensure all staff, including night and weekend shifts, receive equitable exposure to training. Document participation and track metrics for each drill to identify units or staff groups that need additional support.
Technical skill alone does not determine code outcomes. Research consistently identifies communication breakdowns and role confusion as leading contributors to poor resuscitation performance. Every mock code scenario should include deliberate practice of closed-loop communication, clear role assignments, and structured handoffs. During the drill, assign specific roles before the scenario begins: team leader, compressor, airway manager, medication nurse, recorder, and family liaison.
Practicing ACLS team dynamics and communication scripts in simulated scenarios builds the automatic behavioral patterns that hold up under stress. Use your mock code scenarios to identify specific communication failures, such as orders given without acknowledgment, medication dosages not confirmed verbally, or critical interventions not recorded, and address them directly in the debrief.
One of the most frequently cited benefits of in situ mock codes, compared to off-site simulation training, is the ability to identify latent safety threats in your actual environment. These are hazards in the physical space, equipment, or systems that would not be apparent during a classroom training session but surface immediately when a team tries to respond to a code in real time.
During every mock code, include a deliberate equipment check component. Teams should locate and activate the crash cart, confirm defibrillator function, access emergency medications, and operate the overhead paging system. Document any equipment failures, expired medications, missing supplies, or system gaps identified during the drill. These findings should be reported to your quality improvement committee and addressed before the next drill cycle.
Many program designers invest significant resources in creating realistic scenarios but underinvest in the debrief. This is a mistake. Research on simulation-based learning consistently shows that the structured post-event debrief accounts for the majority of learning that occurs during a simulation session. A well-facilitated debrief transforms what teams experienced during the drill into lasting behavioral change.
An effective debrief follows a consistent structure. Begin with a brief factual review of the scenario timeline, then move to a discussion of what the team did well, followed by an honest examination of areas for improvement. The debrief should be psychologically safe: the goal is learning, not blame assignment. Encourage providers to self-identify performance gaps before facilitators point them out. Use objective data from the scenario, such as time to first compression, defibrillation time, and medication timing, to ground the conversation in measurable performance rather than subjective impressions.

The connection between structured debriefing and patient outcomes is well-established. Enhancing patient outcomes through debriefing after ACLS events is a skill that debrief facilitators should develop through formal training. The Debriefing Assessment for Simulation in Healthcare (DASH) tool and the Diamond Debrief Model are two widely used frameworks that can guide facilitator development and standardize your debrief quality across all units.
A mock code program without data is an activity. A mock code program with data is a quality improvement initiative. From the first drill forward, establish a consistent data collection system that captures the following metrics for every simulation: time from recognition of arrest to first compression, time to defibrillation for shockable rhythms, compression rate and depth when technology permits, time to first epinephrine, team role coverage, communication errors observed, and equipment or system failures identified.
Track these metrics longitudinally and compare them to your facility's actual code performance data. Over time, you should see convergence between simulation performance and real-event performance as your team's training becomes internalized. Review your ACLS medications and dosage protocols as part of your regular metric reviews to ensure medication administration accuracy is improving across drill cycles.
Present your program metrics to hospital leadership quarterly. Frame them in terms of patient safety outcomes, accreditation compliance, and risk management. Facilities that can demonstrate documented improvement in code response metrics through simulation training are better positioned for Joint Commission surveys and are building a compelling case for continued program investment. According to research on mock code simulation outcomes, facilities with structured programs consistently outperform those without systematic training initiatives across every measurable resuscitation metric.
Mock code programs perform best when every team member brings a solid foundation of ACLS and BLS knowledge to the simulation. Providers who are current on their certifications arrive at mock codes with the algorithmic knowledge and technical skill baseline that allows them to focus on team performance rather than struggling to recall basic protocols. Keeping your entire team certified is therefore a prerequisite, not an alternative, to mock code training.
For healthcare facilities managing certification across multiple providers, the logistics can be challenging. Affordable ACLS offers group certification solutions for healthcare facilities that allow teams to complete ACLS, BLS, and PALS training online at their own pace, with immediate certification and unlimited retakes. This makes it practical to ensure that your entire code team maintains current certification status without the scheduling disruptions of traditional in-person renewal courses.
Affordable ACLS courses are developed by Board Certified Emergency Medicine physicians and are fully compliant with AHA and ILCOR guidelines. ACLS certification is available for $99, with group pricing options that make facility-wide certification accessible even for smaller clinical practices and community hospitals. When your providers complete their foundational certification through a rigorous online platform, they arrive at your mock code drills ready to apply their knowledge, not just review it.
Beyond technical performance, mock codes serve a critical function in building psychological readiness for high-stress clinical events. Many providers, especially those earlier in their careers, carry significant anxiety about code situations. That anxiety is not irrational, but it can impair performance when left unaddressed. Regular exposure to realistic simulated codes desensitizes providers to the heightened emotional activation of real emergencies and builds the automatic behavioral patterns that allow them to function effectively under acute stress.
For providers who are newer to code team participation, incorporating mental preparation strategies beyond the algorithms into your training program can make a significant difference in how confidently they perform. Your mock code scenarios can include structured reflection exercises, pre-briefing discussions about stress responses, and post-debrief conversations about the emotional experience of resuscitation events. Addressing the psychological dimensions of code response is not a soft skill add-on; it is a clinical performance imperative.
Staff resistance to mock codes is common and understandable. Drills take time away from patient care, create anxiety for some providers, and can feel evaluative rather than educational. The most effective approach to resistance is transparency and psychological safety. Communicate clearly that mock codes are learning opportunities, not performance evaluations. No one fails a mock code. The point is to identify system and team performance gaps so they can be addressed before a real patient's life depends on getting it right. Publishing aggregate, anonymized performance data rather than individual results further reinforces a learning-culture frame. When staff understand that a well-run mock code blue program is designed to support them, not judge them, resistance typically decreases significantly.
Scheduling mock codes in an active clinical environment is genuinely difficult. The most practical approach is to embed drills into existing shift structures rather than creating separate mandatory training sessions. A 20-minute in situ mock code at the beginning of a shift, or during a slower period, is far more achievable than a two-hour off-site simulation event. Designate a pool of trained mock code facilitators from each unit so that drills can be run without depending on the program director's availability for every session. This distributed facilitation model also builds unit-level ownership of the program, which improves both scheduling consistency and staff engagement.
Not every facility has access to high-fidelity simulation manikins or dedicated simulation lab space. Effective mock code programs can be run with low-fidelity manikins, standardized scripts, and minimal equipment. The core value of in situ simulation is the environmental realism and the team interaction, not the sophistication of the manikin. A basic task trainer positioned in an actual patient bed, combined with a well-designed scenario and a skilled debrief, will produce significant learning gains. As your program matures and demonstrates measurable outcomes, building the evidence base for investment in higher-fidelity equipment becomes much more straightforward.
The most effective mock code programs are not isolated training events but components of a broader culture of continuous resuscitation quality improvement. That culture is characterized by regular review of real code data alongside simulation data, transparent discussion of performance gaps at all levels of the organization, ongoing facilitator development and scenario refinement, and leadership that visibly champions simulation-based learning as a patient safety priority.
Facilities that build this culture see compounding returns over time. As team members internalize high-performance behavioral patterns through regular simulation practice, real code events become smoother, more coordinated, and more effective. Staff confidence increases. Hesitation decreases. The gap between what the team knows and what the team does narrows steadily with each drill cycle. The research is unambiguous: institutions that commit to ongoing, structured simulation-based resuscitation training achieve better patient outcomes. That is the fundamental argument for building and sustaining your mock code program.
If your facility is building a mock code program from scratch, start with one unit, measure rigorously, demonstrate outcomes, and expand. If your existing program is inconsistent or underperforming, use the framework in this guide to restructure it around evidence-based principles. The investment in time and resources is significant, but the potential return, measured in lives saved, is incalculable.
Building an effective mock code program requires commitment, coordination, and a willingness to examine performance gaps honestly and systematically. It also requires that every member of your code team brings current, high-quality ACLS and BLS certification to the simulation environment. Without that foundational knowledge base, mock codes cannot achieve their full potential.
Affordable ACLS makes it simple for healthcare facilities of all sizes to keep their providers certification-current with 100% online, self-paced ACLS, BLS, and PALS courses developed by emergency medicine physicians and fully compliant with current AHA and ILCOR guidelines. Group pricing options, immediate digital certification, and unlimited retakes remove the traditional barriers to maintaining facility-wide certification compliance. Visit affordableacls.com or call 866-655-2157 to learn more about certification solutions for your team.
Your patients deserve a code team that performs as well in real emergencies as they do in the best-case scenario. A well-designed mock code program, supported by current individual certifications, is how you build that team. The next code blue in your facility will not announce itself in advance. Build your program today so your team is ready when it happens.
.jpg)

