Every minute without circulation during cardiac arrest causes irreversible damage to the brain and vital organs. Despite decades of refinement in conventional CPR techniques, defibrillation protocols, and advanced cardiac life support algorithms, a significant proportion of cardiac arrest patients never achieve a sustained return of spontaneous circulation. For these patients — those with refractory cardiac arrest — a new frontier of resuscitation has emerged: Extracorporeal CPR, or ECPR.
ECPR represents one of the most significant advances in emergency resuscitation medicine in the last two decades. By deploying extracorporeal membrane oxygenation (ECMO) technology during active resuscitation, ECPR effectively takes over the work of the heart and lungs, buying critical time for the underlying cause of arrest to be identified and treated. For healthcare professionals working in emergency departments, cardiac care units, and critical care environments, understanding ECPR — how it works, who qualifies, and what the evidence shows — is increasingly essential knowledge. This technology, combined with a broader wave of innovation, reflects the remarkable evolution covered in our overview of advancements in cardiology that are reshaping how clinicians approach heart disease and arrest management.
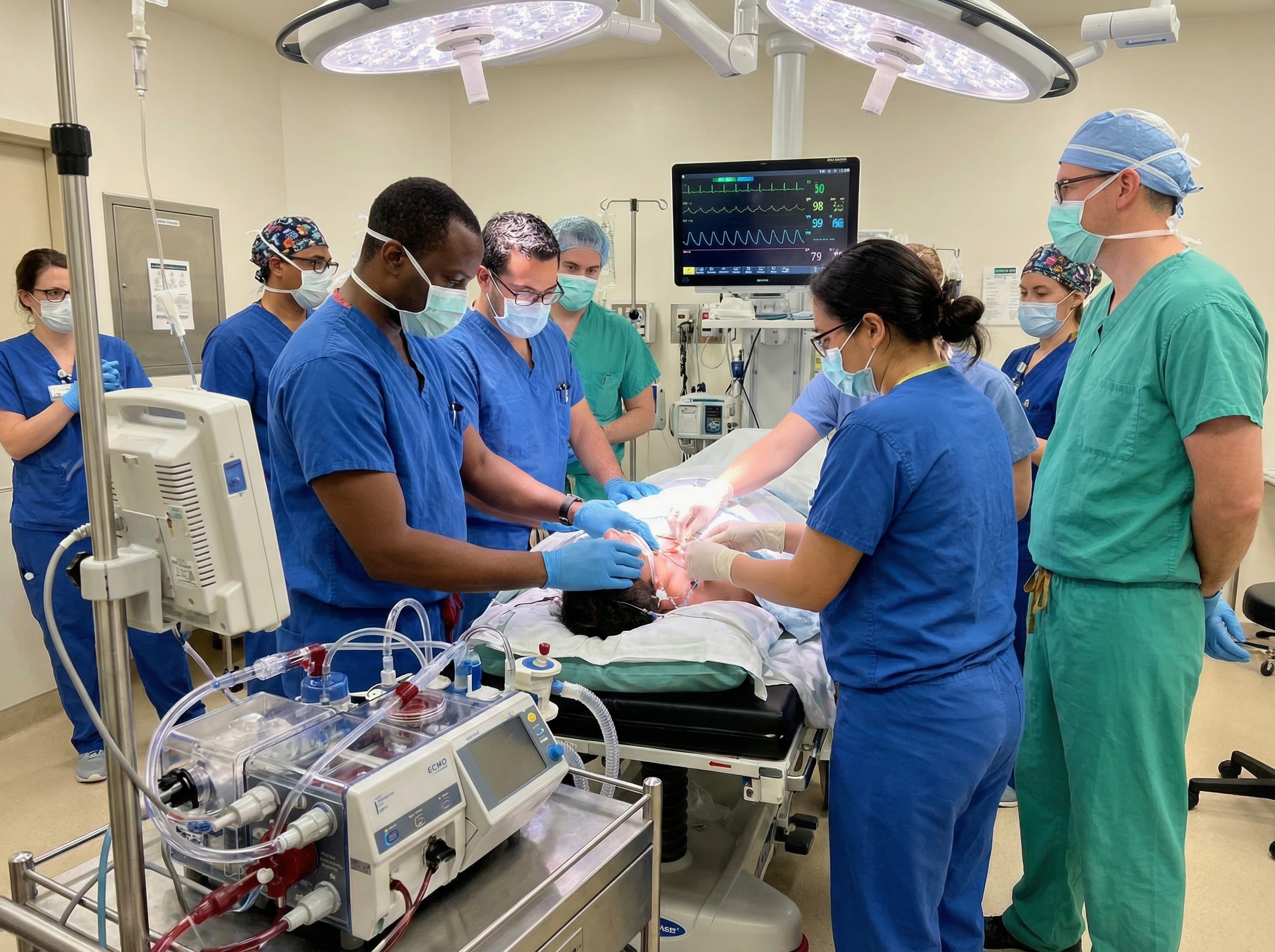
Extracorporeal CPR is defined as the use of extracorporeal membrane oxygenation in patients who have not achieved return of spontaneous circulation (ROSC) despite standard advanced cardiac life support (ACLS) measures. In other words, ECPR is initiated when conventional resuscitation has failed or is unlikely to succeed within a medically acceptable timeframe.
At the heart of ECPR is venoarterial ECMO (VA-ECMO). This technology involves placing large cannulas — typically in the femoral vein and femoral artery — through which blood is drained from the venous system, oxygenated and cleared of carbon dioxide by an external membrane oxygenator, and then returned under pressure to the arterial circulation. The result is a mechanical bypass of both the heart and lungs, maintaining systemic perfusion pressure and oxygenation even when the heart is unable to pump.
The distinction between ECPR and standard ECMO use is important. ECMO is routinely used in cardiac surgery and for patients in cardiogenic shock as a bridge to recovery or transplant. ECPR specifically refers to ECMO deployment during active cardiac arrest as part of the resuscitation effort itself — a significantly more urgent, time-pressured, and technically demanding application. Familiarity with the adult cardiac arrest circular algorithm is essential context for understanding where ECPR fits within the broader resuscitation framework.
The clinical evidence for ECPR has grown substantially over the past decade, and the results are compelling when compared to historical survival rates for refractory cardiac arrest.
Conventional out-of-hospital cardiac arrest (OHCA) carries dismal survival odds — typically under 10% in most regions, with neurologically intact survival even lower. Refractory cardiac arrest, defined as arrest that persists despite 20 or more minutes of conventional CPR, carries survival rates approaching zero with standard resuscitation alone. Against this backdrop, ECPR outcomes are striking. According to data from the Extracorporeal Life Support Organization (ELSO) registry, more than 15,000 ECPR cases have been documented, with an overall survival to hospital discharge rate of approximately 29-30%. That represents a three- to four-fold improvement over conventional care for the same patient population.
Perhaps even more encouraging is the trajectory of outcomes as programs mature. Neurologically favorable survival rates improve as institutions accumulate experience and standardize their protocols. The Vienna eCPR program reported favorable neurologic outcomes increasing from 15% in 2020 to 37% by 2023 — a more than doubling of meaningful survival over just four years. As documented in Annals of Emergency Medicine, outcomes in ECPR programs consistently improve with center experience, reflecting the importance of training, patient selection refinement, and operational standardization.
Timing is the single most critical variable in ECPR outcomes. Research consistently shows that ECMO flow established within 20 minutes of conventional CPR initiation yields the best results — survival rates up to 30% at this threshold. Beyond 40 minutes of low-flow conventional CPR prior to ECMO initiation, outcomes deteriorate significantly, with diminishing probability of meaningful neurologic recovery even if ECMO is technically successful. This urgency fundamentally shapes how ECPR programs are designed and operated.
Not every patient in refractory cardiac arrest is a candidate for ECPR. The intervention requires significant resources, carries substantial risks, and is most beneficial when applied to a carefully selected population. While universally accepted criteria do not yet exist — and guidelines continue to evolve — several key factors guide patient selection across most established programs.
The optimal ECPR candidate shares a common profile: relatively young age (most protocols set an upper limit between 65 and 75 years, with American Heart Association guidance suggesting under 75 as reasonable), minimal or no no-flow time before CPR initiation, a shockable initial rhythm, a potentially reversible cause of arrest, and the ability to achieve vascular access and ECMO flow within 60 minutes of arrest onset. Patients with prolonged no-flow times, non-shockable rhythms, significant comorbidities limiting functional recovery, or non-survivable underlying conditions are generally not ideal candidates.
The significance of initial cardiac rhythm cannot be overstated. Shockable rhythms like ventricular fibrillation and pulseless ventricular tachycardia represent electrical disorganization of a heart that may be structurally salvageable — making these patients the strongest candidates for ECPR. In contrast, non-shockable rhythms like pulseless electrical activity (PEA) or asystole often reflect more severe myocardial damage or systemic pathology that limits the likelihood of recovery even with circulatory support. Understanding the causes and treatment of PEA is essential context for clinicians evaluating ECPR candidacy.
Identifying a reversible cause of arrest is fundamental to ECPR candidacy assessment. The well-established Hs and Ts framework used in ACLS — covering causes from hypoxia and hypovolemia to tension pneumothorax and thrombosis — serves as the backbone for this evaluation. Patients whose arrest stems from a treatable cause such as massive pulmonary embolism, acute myocardial infarction, severe hypothermia, or toxic ingestion have the greatest potential for meaningful recovery when circulatory support is provided. Reviewing the Hs and Ts of sudden cardiac arrest is a critical competency for any clinician involved in ECPR triage decisions.
Executing ECPR successfully requires a choreographed, multidisciplinary team response that must unfold with precision and speed. Unlike conventional ACLS, which can be delivered by a trained provider with basic equipment, ECPR demands a highly coordinated team, specialized equipment, and institutional infrastructure.
A functional ECPR team typically includes an emergency physician or intensivist capable of performing emergency ECMO cannulation, perfusionists or trained nurses to operate the ECMO circuit, additional providers to maintain high-quality conventional CPR during cannulation, and support staff to prepare and prime the circuit. The role of each team member must be predefined, practiced, and immediately deployable — because in ECPR, seconds genuinely matter.
While resuscitation continues — including chest compressions and standard ACLS medications — the cannulation team accesses the femoral vessels using ultrasound guidance. Wire access, vessel dilation, and cannula placement proceed in parallel with ongoing CPR. Once both cannulas are placed and the circuit is connected and primed, ECMO flow is initiated. The goal is to achieve adequate ECMO flow — typically 4-6 liters per minute — as rapidly as possible. The pharmacologic components of this process, including appropriate use of ACLS medications, are well detailed in the ACLS medications cheat sheet covering dosages, routes, and indications.
Once ECMO flow is established, the patient is typically transferred to the cardiac catheterization laboratory or intensive care unit for definitive evaluation and treatment of the underlying cause. Coronary angiography and percutaneous coronary intervention are performed if myocardial infarction is suspected. Thrombectomy or thrombolytics are deployed for pulmonary embolism. Hypothermic patients undergo controlled rewarming using the ECMO circuit's heat exchanger — one of the unique advantages of ECMO in this context, as it allows precise temperature management.
Survival to ECMO initiation is only the beginning. Post-ECPR care is complex and intensive, requiring the same rigorous attention to post-cardiac arrest management principles that apply to all resuscitated patients — but with the added complexity of managing an ECMO circuit, anticoagulation, and the underlying condition driving the arrest.
Targeted temperature management (TTM) is an important component of post-ECPR care. The ECMO circuit's oxygenator includes a heat exchanger capable of precisely controlling patient temperature — a significant advantage over conventional cooling methods. Current recommendations support targeting 33-36 degrees Celsius for 24 hours followed by controlled rewarming to 37 degrees Celsius, mirroring standard post-cardiac arrest care guidance. This neuroprotective strategy aims to reduce secondary brain injury from reperfusion.
Hemodynamic optimization on ECMO requires careful attention to ECMO flow rates, vasopressor support, fluid balance, and oxygenation targets. Clinical guidelines recommend targeting arterial oxygen saturation of 92-97% to avoid both hypoxia and hyperoxia, both of which can worsen neurologic outcomes. The principles underlying immediate post-cardiac arrest care apply fully in the ECPR context, with the added layer of ECMO management. Clinicians should also be familiar with the comprehensive guidance on post-ROSC care to understand what happens after the heart begins beating again following resuscitation.
ECMO weaning is initiated when cardiac function shows signs of recovery — evidenced by improving echocardiographic function, improving pulse pressure on arterial waveform, and hemodynamic stability at reduced ECMO flow rates. Successful weaning, followed by decannulation and transfer out of intensive care, represents the best possible trajectory. When cardiac recovery does not occur despite optimal management, ECMO may serve as a bridge to durable mechanical circulatory support or cardiac transplantation in appropriate candidates.
Establishing a functional ECPR program is not a minor undertaking. It requires institutional commitment, specialized equipment, trained personnel, clearly defined protocols, and a culture of continuous quality improvement. According to peer-reviewed research on ECMO for cardiac arrest, the most successful ECPR programs are built upon foundations of high-volume ECMO experience — institutions that are already proficient in ECMO for other indications before extending its use to the cardiac arrest setting.
Team training is a critical success factor. International consensus guidance from the Extracorporeal Life Support Organization specifies knowledge and curriculum requirements, skill prerequisites, and competency standards for ECPR practitioners. Research has shown that emergency medicine residents given structured training using instructional videos and hands-on ECMO equipment can achieve a 75% success rate in ECPR initiation in simulation environments — demonstrating that training is achievable but must be deliberate and systematic. This mirrors the broader shift toward simulation-based education described in our article on technological innovations transforming ACLS training.
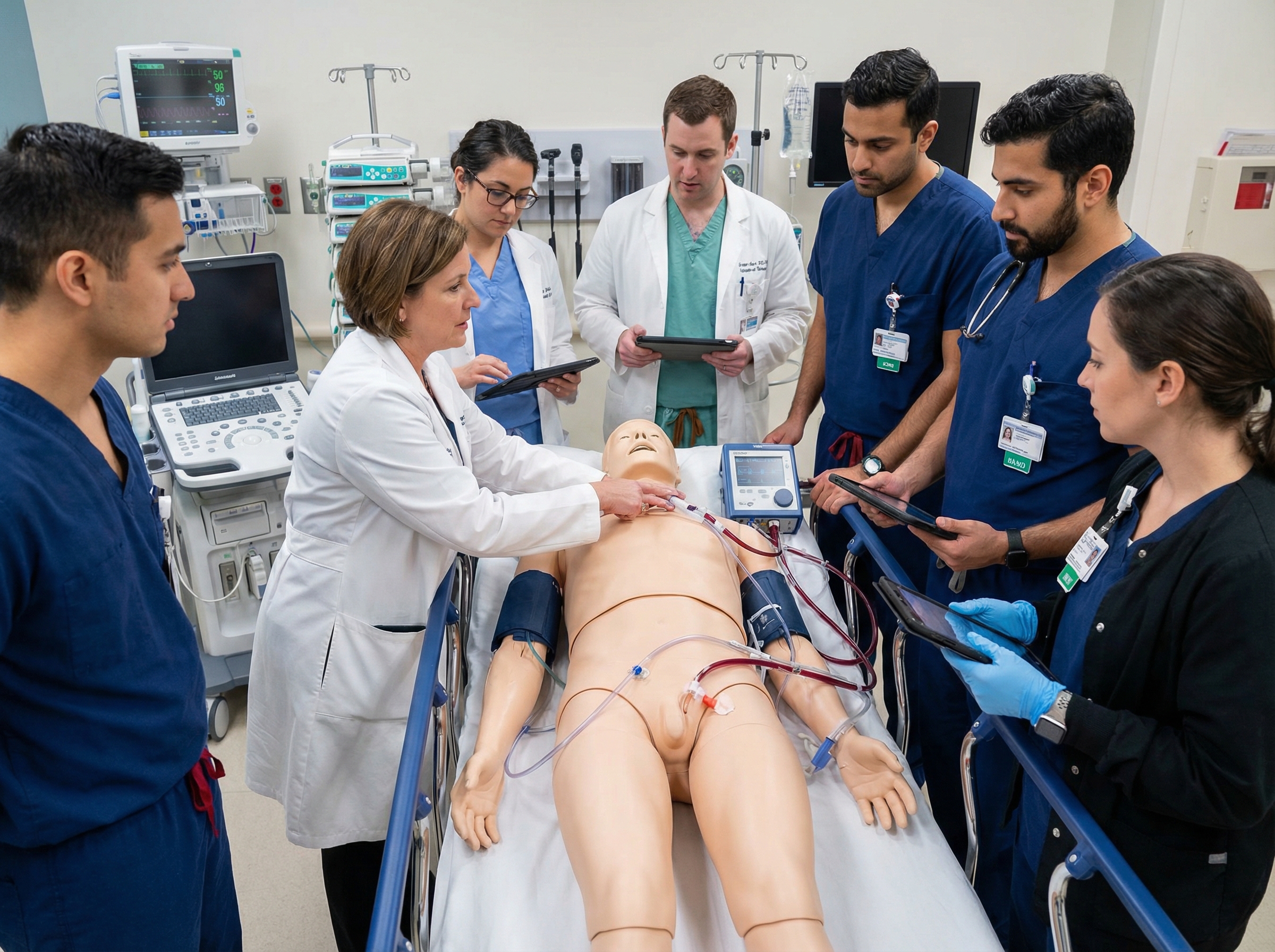
High-fidelity simulation training is increasingly recognized as essential for ECPR team preparation. Teams must rehearse the entire ECPR activation sequence — from alert to cannulation to ECMO initiation — repeatedly and under realistic conditions to build the muscle memory and communication patterns that enable rapid, safe execution under the extreme time pressure of real cardiac arrest. Programs that track key performance metrics including time from arrest to ECMO initiation, cannulation success rates, complication rates, survival to discharge, and neurologically favorable survival consistently demonstrate better outcomes over time.
The ELSO interim guideline consensus statement for ECPR in adults provides a valuable framework for institutions building new programs, covering equipment specifications, team structure, patient selection criteria, and quality metrics. Adherence to these guidelines has been associated with improved neurologic outcomes across multiple studies, reinforcing the value of standardized, evidence-based program design.
Despite its promise, ECPR is not without significant challenges and limitations that must be honestly acknowledged by any institution considering its implementation.
Resource intensity is the most immediate barrier. ECMO circuits, cannulas, oxygenators, and associated equipment represent substantial capital investment. Maintaining a 24/7 capable ECPR team requires staffing commitments that are difficult for many hospitals to sustain. ECMO is among the most resource-intensive interventions in all of hospital medicine, and its application during cardiac arrest — when decisions must be made in minutes under extreme pressure — amplifies these demands considerably.
Patient selection remains one of the field's greatest challenges. The absence of universally accepted criteria means that different institutions apply different eligibility standards, making outcome comparisons across programs difficult. Over-inclusive selection leads to ECMO use in patients unlikely to benefit, consuming resources and potentially prolonging suffering. Under-inclusive selection means some patients who might survive are denied the intervention. Ongoing randomized controlled trials are generating the evidence needed to refine selection standards, and clinicians should stay current with the key changes in ACLS guidelines for 2025 as this field continues to evolve.
Geographic access and equity are also significant concerns. ECPR is currently available only at a limited number of specialized centers, meaning that geography substantially determines whether a patient has access to this potentially life-saving technology. Emerging pre-hospital ECPR programs — where trained mobile teams bring ECMO to the field — represent a promising approach to extending access, but these programs face their own implementation challenges related to cost, training, and logistics.
Procedural complications including vascular injury, limb ischemia, bleeding, and stroke are real risks that must be weighed against the potential benefit. Anticoagulation requirements for ECMO circuit management create ongoing bleeding risk, particularly in a post-cardiac arrest patient who may have received thrombolytics or who has concurrent coagulopathy. Multiorgan failure following prolonged cardiac arrest can limit recovery even when ECMO successfully restores circulation.
The trajectory of ECPR development points toward expanding access, improving patient selection through better biomarkers and predictive tools, and generating higher-quality evidence from randomized controlled trials. The field is moving rapidly, and the next five to ten years are likely to see substantial advances.
Pre-hospital ECPR — deploying ECMO in the field by specially trained emergency medical teams — has been piloted in several European and North American centers. Early results suggest that pre-hospital ECPR can reduce the critical time interval between arrest and ECMO initiation, potentially improving outcomes for out-of-hospital cardiac arrest patients who would otherwise not survive transport. As published in research on improving ECPR access, pre-hospital delivery and regional ECPR networks represent key strategies for extending access beyond specialized tertiary centers.
Artificial intelligence and machine learning tools are being developed to assist with real-time ECPR candidacy assessment, analyzing cardiac rhythm, arrest characteristics, patient demographics, and clinical context to predict likelihood of meaningful recovery. If validated, these tools could improve both the speed and accuracy of patient selection decisions — one of the critical bottlenecks in ECPR activation.
The field is also awaiting results from ongoing randomized controlled trials that will provide the highest level of evidence for or against ECPR in specific patient populations. The ARREST trial, which demonstrated improved survival in refractory ventricular fibrillation, and the Prague OHCA trial have been landmark contributions, but the evidence base is still developing. Higher-quality data will allow clearer guideline recommendations and greater confidence in program expansion decisions. As published in The Lancet Respiratory Medicine, the evolving evidence for ECPR in refractory cardiac arrest continues to shape how programs and guidelines approach this intervention.
ECPR represents a paradigm shift in how we think about the limits of cardiac resuscitation. For the majority of practicing emergency physicians, intensivists, cardiologists, and critical care nurses, ECPR will not be a routine intervention — but understanding its principles, indications, and limitations is increasingly important for clinical practice and for providing accurate information to patients and families.
For all healthcare providers, mastery of conventional ACLS remains the essential foundation. ECPR does not replace excellent high-quality CPR, timely defibrillation, appropriate ACLS medications, and systematic identification and treatment of reversible causes — it extends these fundamentals for the subset of patients who do not respond to them. Real-world outcomes illustrate this principle repeatedly: high-quality conventional resuscitation saves the majority of salvageable patients, and ECPR serves the critical remainder. Reading about real-life ACLS cases that made a difference underscores how foundational skills remain decisive in cardiac arrest outcomes.
Whether you are a seasoned emergency physician exploring ECPR program leadership or a nurse seeking to refresh your ACLS certification to better support your resuscitation team, ongoing education is non-negotiable in this rapidly evolving field. Affordable ACLS offers comprehensive, 100% online ACLS certification and recertification developed by board-certified emergency medicine physicians — covering cardiac arrest algorithms, post-arrest care, medications, airway management, and the clinical reasoning skills that underpin advanced resuscitation practice. With self-paced learning, unlimited retakes, and immediate certification upon completion, Affordable ACLS makes it easier than ever for busy clinicians to stay current.
Extracorporeal CPR represents one of the most exciting and consequential developments in resuscitation medicine in recent history. For patients whose hearts fail to respond to even the best conventional care, ECPR offers a legitimate second chance — and with outcomes improving as programs mature and evidence accumulates, that chance is becoming more meaningful each year.
The technology, the evidence, and the operational frameworks for ECPR are all advancing rapidly. Clinicians who invest in understanding this intervention — its mechanisms, its patient selection criteria, its implementation requirements, and its limitations — will be better positioned to advocate for appropriate patients, contribute to institutional program development, and deliver the highest possible standard of care in the most critical moments. In cardiac arrest resuscitation, knowledge is as essential as any piece of equipment, and ECPR is becoming an increasingly essential part of that knowledge base.
Ready to build the clinical foundation that supports advanced resuscitation practice? Visit Affordable ACLS to explore our ACLS, BLS, and PALS certification courses — designed by emergency physicians for the realities of modern clinical practice, available entirely online, and priced to make excellence in resuscitation accessible to every healthcare professional.
.jpg)

